Since this is not an unusual finding, but there is little scientific literature on it, I will dedicate today’s post to dystrophic calcifications in chronic venous ulcers.
When we speak of calcifications we are referring to abnormal deposits of insoluble calcium salts. When they are arranged in an organized way forming bone, they are called ossifications.
Calcinosis cutis is the term used when this calcification occurs in the skin tissue and can be classified as follows (Urbina, 2001):
- Dystrophic calcification, due to tissue damage secondary to trauma, burns and inflammatory, degenerative or neoplastic diseases.
- Metastatic calcification, associated with various disorders that occur with elevated plasma levels of calcium and /or phosphorus.
- Idiopathic calcification, which is not related to tissue damage or metabolic disorders.
The most frequent group is dystrophic calcifications. Among the inflammatory causes is chronic venous insufficiency, with or without the presence of a cutaneous ulcer. Calcium-phosphorus metabolism and serum levels are normal. Different hypotheses have been proposed to explain the development of these ectopic calcifications. Anoxia and inflammation that occur in the legs with venous hypertension involves cell necrosis and the release of cells and inflammatory mediators, with the production of free radicals and damage to connective tissue (collagen, elastin) or subcutaneous fat. In this damaged tissue, intracellular calcium levels may increase, with the consequent formation and precipitation of crystals. On the other hand, denatured proteins bind to phosphate and allow them to bind to calcium, with consequent precipitation of calcium phosphate.
The diagnosis can be made by palpation and visualization in radiography or ultrasound (Piry, 1992).
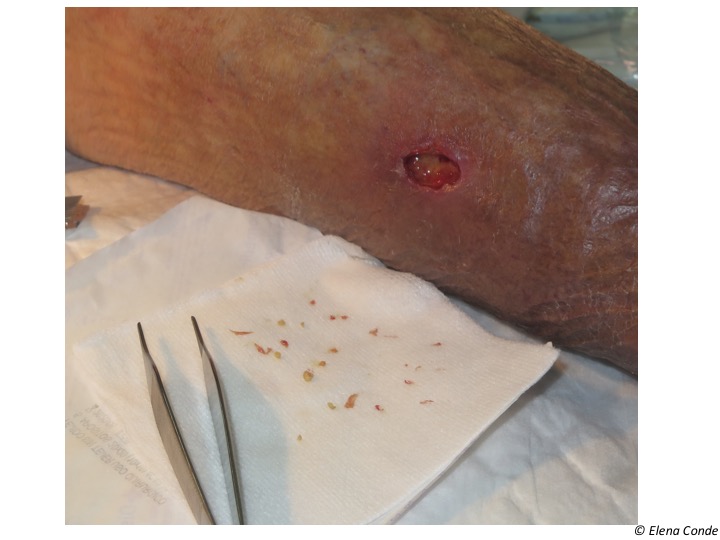
When the patient presents a cutaneous ulcer, this calcification can become visible, as a hard material of bone consistency and dark brown coloration. Normally they are strongly adhered to the wound bed, with significant pain when trying to pull on them. These deposits act as a foreign body, which promotes the inflammatory response in the wound and therefore slows healing. A retrospective study of 212 patients with chronic leg ulcers (no response to conventional treatment for at least 3 months) found calcifications in 18% and ossifications in 7% of patients. The presence of these abnormal deposits was associated with greater pain and worse response to compressive treatment (Wollina, 2009).
The main radiological differential diagnosis has to be made with phlebolites, which correspond to parietal venous calcifications after episodes of deep vein thrombosis.
There are different options in the treatment of these ossifications in skin ulcers, but all involve their removal from the wound bed (Chaverri, 2011; Enoch, 2005):
- Achieve detachment of calcification by moisturizing the wound bed with hydrogel-type dressings
- Mechanical removal with tweezers and scalpel. Since it is painful, it is recommended to previously anaesthetize the area.
- Surgical excision under anaesthesia
- Radical debridement of the ulcer, with or without subsequent coverage with skin graft.
Referencias:
- Chaverri Fierro D, Portas Freixes J, Bosch Cuenca M, Sáez Horts M, Montoya Hellín I, González Sierra M et al. Calcificación distrófica en úlceras de la extremidad inferior. Gerokomos 2011; 22 (3): 126-130.
- Enoch S. Kupitz S, Miller DR and Harding KG. Dystrophic calcification as a cause for non healing leg ulcers. Int Wound J 2005; 2:142-147.
- Piry A, Vin F, Allaert FA. Inflammation and subcutaneous calcification of venous origins. Fhlebologie 1992; 45 (1): 41-7.
- Urbina F, Pérez L, Sudy E, Misad C. Calcificación y osificación cutánea. Actas Dermosifiliogr. 2001;92:255-69.
- Wollina U, Hassenöhrl K, Köstler E, Schönlebe J, Heinig B, Haroske G, Kittner T, Dystrophic calcification in chronic leg ulcers – a clinocopathologic study. Dermatol Surg 2009; 35(3): 457-61.
Also available in: Español (Spanish)






