“How do you cover the donor site?“ This is a question that always arises when I talk about the punch grafting technique that we do in our clinic. And it is an essential question, since we have to optimize the care of that new wound that we have generated in order to heal another one. Our priorities are to avoid pain, control bleeding, exudate and to favour a fast complete epithelialization.
The idea of writing this post came to me when I read a recent review of dressings used in the donor site.1
Before continuing, as a reminder, the most widespread type of partial thickness skin graft is the mesh graft obtained with dermatome. However, in our practice, where we treat predominantly leg wounds, we use punch grafting (See post: “Types of grafts to cover chronic wounds: which one should you choose“). The grafts can be obtained with a punch, scalpel blade or curette.
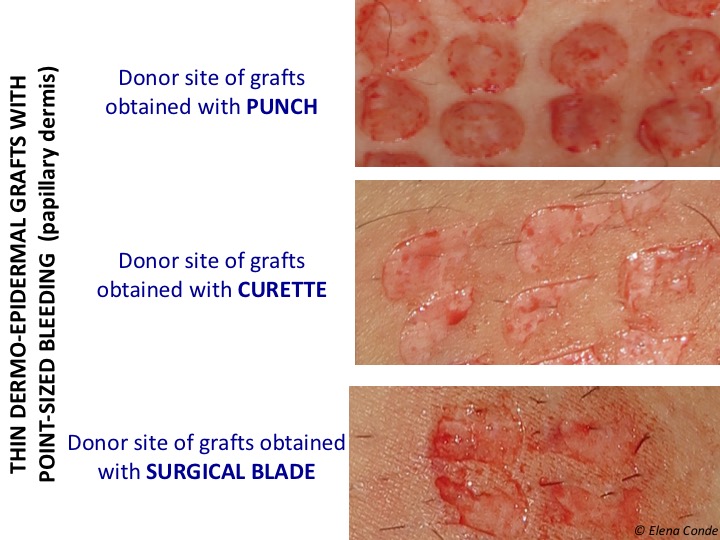
The bleeding in the three cases will be point-sized because we reach papillary dermis (see post: “Differences between epidermal grafts and dermo-epidermal punch grafts“). The presence of multiple free nerve endings in the dermo-epidermal junction, which are exposed or damaged after obtaining the thin skin graft, explains pain in the donor site.
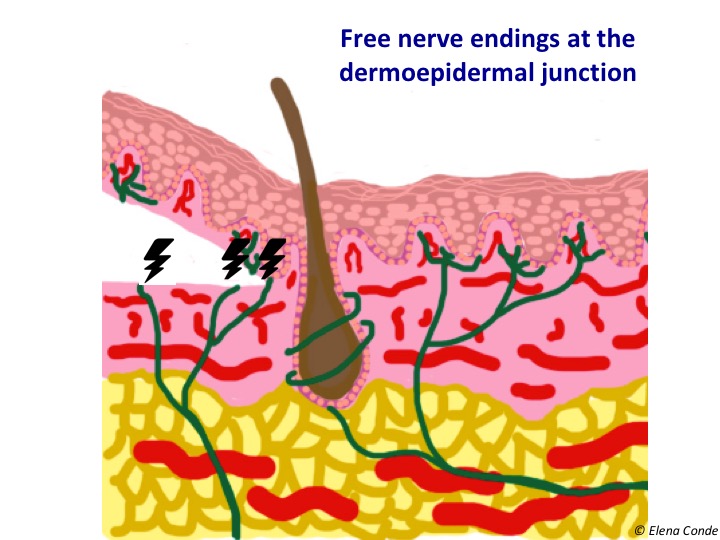
Despite the different techniques for obtaining thin split-thickness skin grafts, the recommendations for management of the donor site are valid for all of them.
Since there is no consensus and, depending on the wound clinic, the protocol of care of the donor site may vary, let’s first see what the studies say. Later, I will tell you what we do in our wound clinic.
Let’s go back to the review1 that was designed to answer the interesting question: which dressing is most effective in reducing pain and accelerating healing of the graft donor site? Thirty-five articles (from clinical trials to case series) were included in the review. All studies used pain scales, but the type of scale and timing of measurement was highly variable. None of the studies detailed the analgesic drugs used, an essential variable in this type of studies. The definition of complete healing also varied between studies. Returning to the objective question of the review, and taking into account the limitations of the study in making comparisons, no dressing has shown superiority. However, interesting conclusions can be drawn from this review:
- Most papers comparing dry healing with the use of dressings designed to maintain a moist environment in the wound bed, find better pain control and faster healing in the second group.
- Although a dressing may provide a higher pain reduction in the first few days after the procedure, its power of absorption and the consequent frequency of dressing changes required until complete epithelialisation must be taken into account. For example, a clinical trial2 comparing polyurethane film with alginate underlines that, although the former shows a greater initial analgesic effect, haemostatic power and exudate management with fewer dressing changes makes alginate an interesting alternative, even though there are no significant differences in time to complete epithelialization (21.9 days in the polyurethane film group vs. 18.8 in the alginate group).
- The secondary dressing is also important to regulate the wound microenvironment and is not usually detailed in the studies.
- As the healing process evolves, it would be interesting to change the type of dressing, depending on the needs of the wound and the patient, always prioritizing comfort.
“Rapid epithelialization and pain control” should be our goal with the donor site. Before focusing on our experience, I am going to comment on a very interesting strategy that has just been published: mincing the remains of the laminar graft into very small fragments (wounds are irregular and there is usually excess tissue from the graft), uniformly spreading them on the entire surface of the donor site, prior to covering it with a calcium alginate dressing.3 The authors present a clinical trial including 96 patients. An average reduction of 4 days was found until complete epithelialisation (9.1 days in the treatment group and 13.1 days in the control), regardless of the size of the donor site. The benefit in epithelialization may be associated with keratinocytes, growth factors and other cytokines released onto the wound bed. In fact, this is the behaviour that may also have the punch grafts that are observed to accelerate healing despite not achieving appropriate graft taking in the wound bed. Undoubtedly, the excellent proposal of these authors is a very efficient way not to waste tissue!
And now, welcome to our wound clinic! This is the operating table with the material necessary to obtain the grafts (in this case with scalpel blade) and cover the donor site. We use calcium alginate dressing as a primary dressing (which we usually apply in several layers) and gauze with adhesive as a secondary dressing. We always try to place the dressings under local pressure.
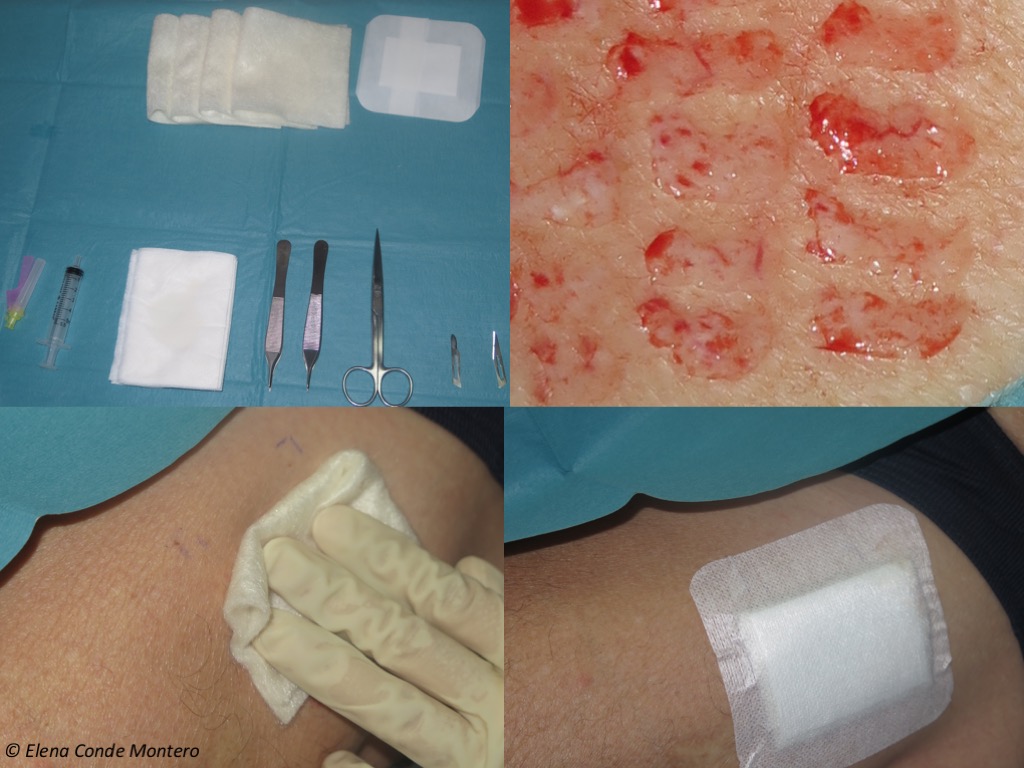
Sometimes, in the first dressing changes, which we always try to space out as much as possible, patients refer pruritus in the donor site. When the alginate dressing is removed, always carefully (if it is stuck we moisten it to get an atraumatic detachment), we may find bright erythema and oedema limited to the donor site.
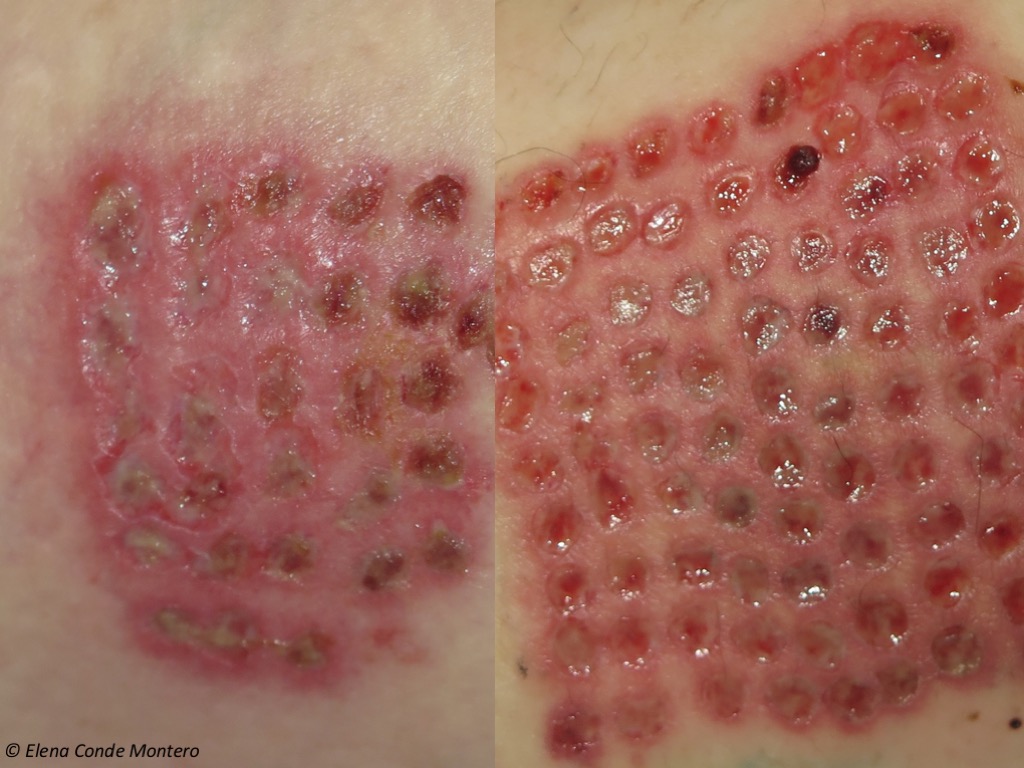
This inflammatory reaction is managed by increasing the frequency of dressing changes and applying topical corticosteroid cream. If this reaction arises early and the wound bed is exudative and still needs alginate coverage, in each dressing changes we apply gauzes soaked with a corticosteroid solution, and leave them on the wound bed for some minutes. When the majority of wounds are in the final scab phase, the patient can apply a moderate potency corticoid cream at night for 5-7 days, without the need for dressing coverage.
In a preventive way, since its appearance is more frequent when we perform grafts in large areas or if the patient has presented this reaction in previous procedures, we apply gauzes soaked with the corticoid solution immediately after obtaining the grafts.
If there is no more bleeding and the wounds are covered by scab, there are different options to accelerate epithelialization and reduce discomfort in the area. One of them is to apply repairing creams with hyaluronic acid (see post “Reasons for the hyaluronic acid boom in wound healing“), zinc (see post “Why we use topical zinc in wounds and perilesional skin“) or other pro-cicatrizing and anti-inflammatory active principles until complete epithelialization (normally in 2-3 weeks), at which time the patient would begin to apply his usual emollient cream.

This is an example of the typical clinical appearance of the donor site on the day of the procedure, at 2 weeks, 3 and 6 months later. The scar is usually not palpable and its final coloration depends on the phototype, the age of the patient and the duration of the inflammatory process until healing (the shorter, the better aesthetic results).
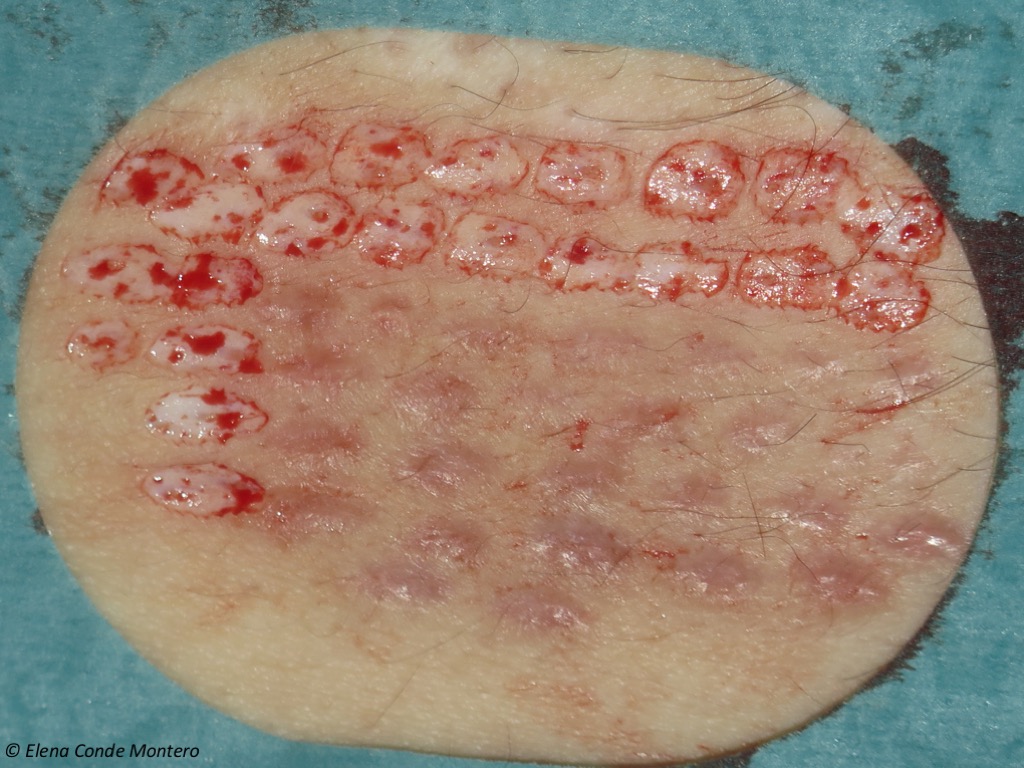
On many occasions we graft wound beds that are not optimal, so we may need to repeat the procedure several times. This is not a problem for patients, since punch grafting is a very well accepted and tolerated technique, which we perform in the consultation room. This is an example of a donor site from which grafts have just been obtained, adjacent to a scar area where the procedure had been performed a few months earlier.
This is our experience. What coverage of the donor site do you prefer?
References:
Also available in: Español (Spanish)






