
Pustular and erosive dermatosis of the legs is a disorder that may be underdiagnosed because of lack of knowledge of its existence.. Have you ever heard of it? Probably, after reading this post, some case will come to your mind that could be framed in this diagnosis. Here we go.
What is pustular and erosive leg dermatosis?
It is an inflammatory entity of unknown origin. The first description was made by Laningan in 1987.1 Since then, isolated cases and some short case series have been published.2 Its incidence is underestimated since diagnosis is not usually made due to lack of knowledge of the disorder. Pustular and erosive dermatosis can also appear on the scalp.
It usually affects older women. Despite the fact that sometimes non-follicular pustules of variable size and friable consistency may be seen, it is common that erosions predominate, with or without scabs. It frequently occurs in the context of chronic venous insufficiency. The involvement can be uni or bilateral, especially in the anterior central aspect of the of the legs. The lesions are painless and itching is not frequent. The clinical course is progressive and does not ameliorate spontaneously. The fact that in most cases we do not observe the pustules, may hinder the diagnosis of this cutaneous disorder.2,3
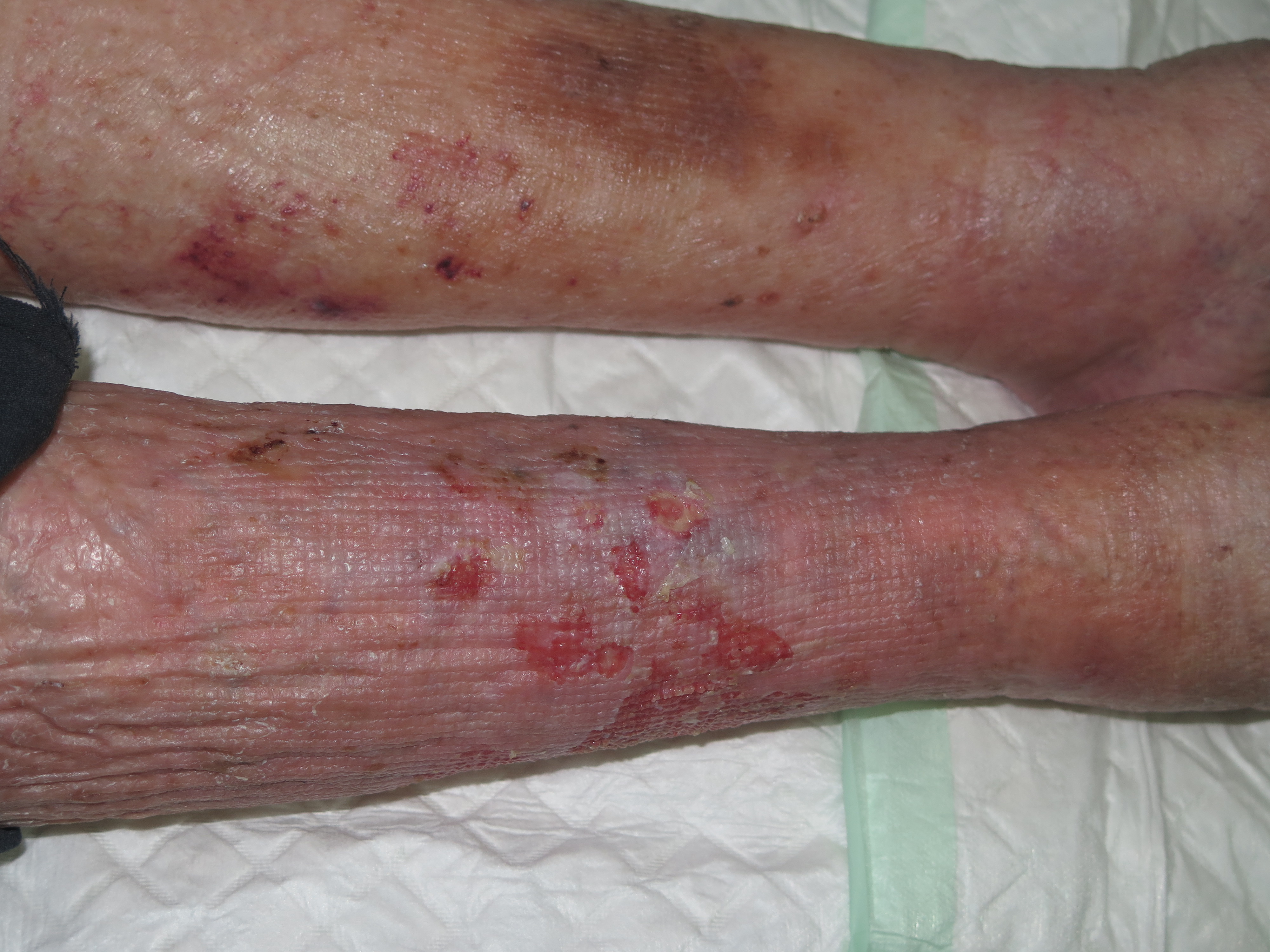
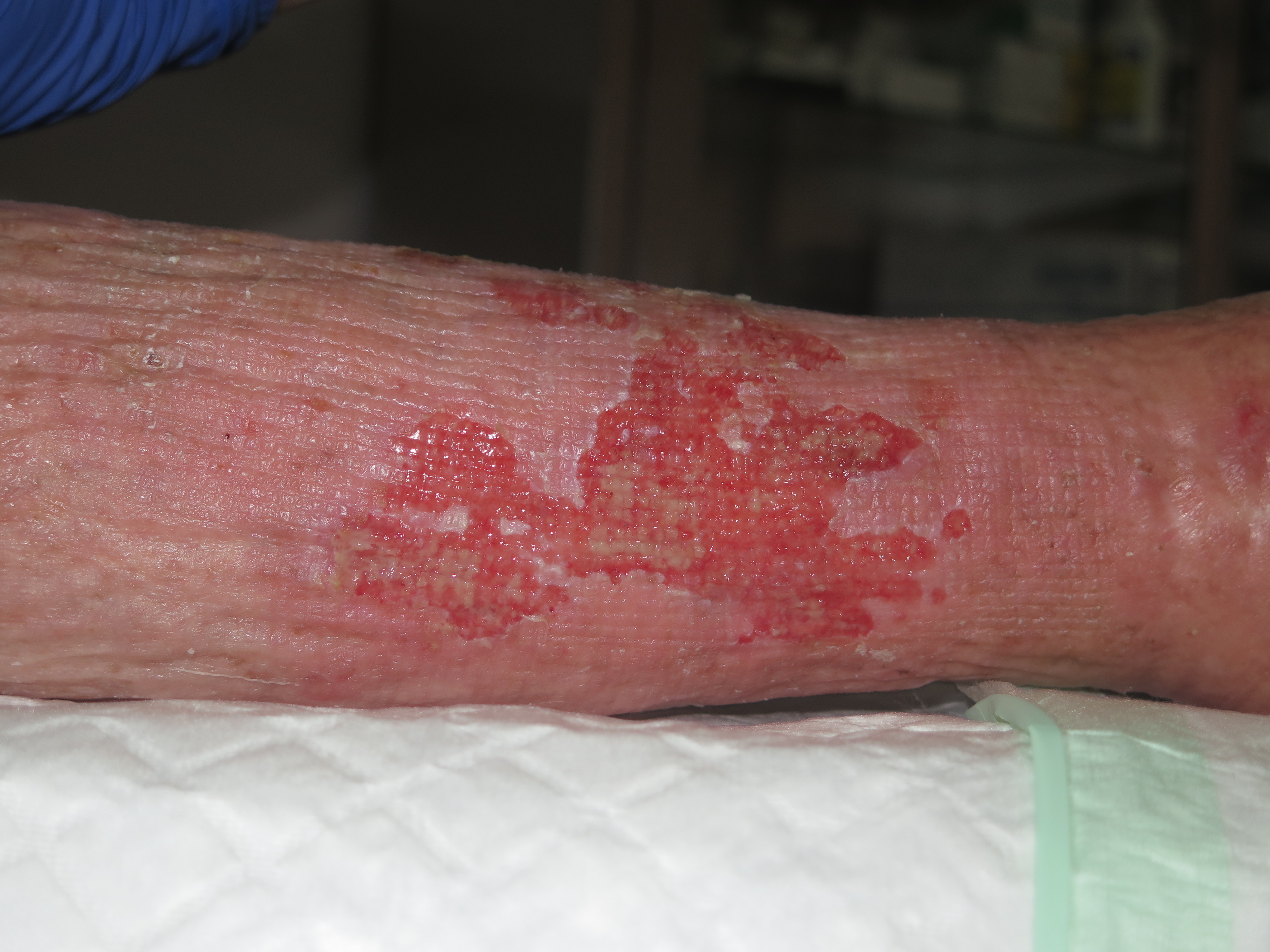
Why does it happen?
Its etiopathogenesis is unclear. It would be included in the spectrum of inflammatory diseases. Some authors consider it a neutrophilic dermatosis.
Possible predisposing factors include:
- Cutaneous atrophy due to photoaging
- Chronic venous insufficiency
- Chronic skin inflammation
- Wounds (ulcers, graft or donor sites, burns, trauma)
- Occlusion with bandages or dressings
- Zinc, vitamin C deficiency
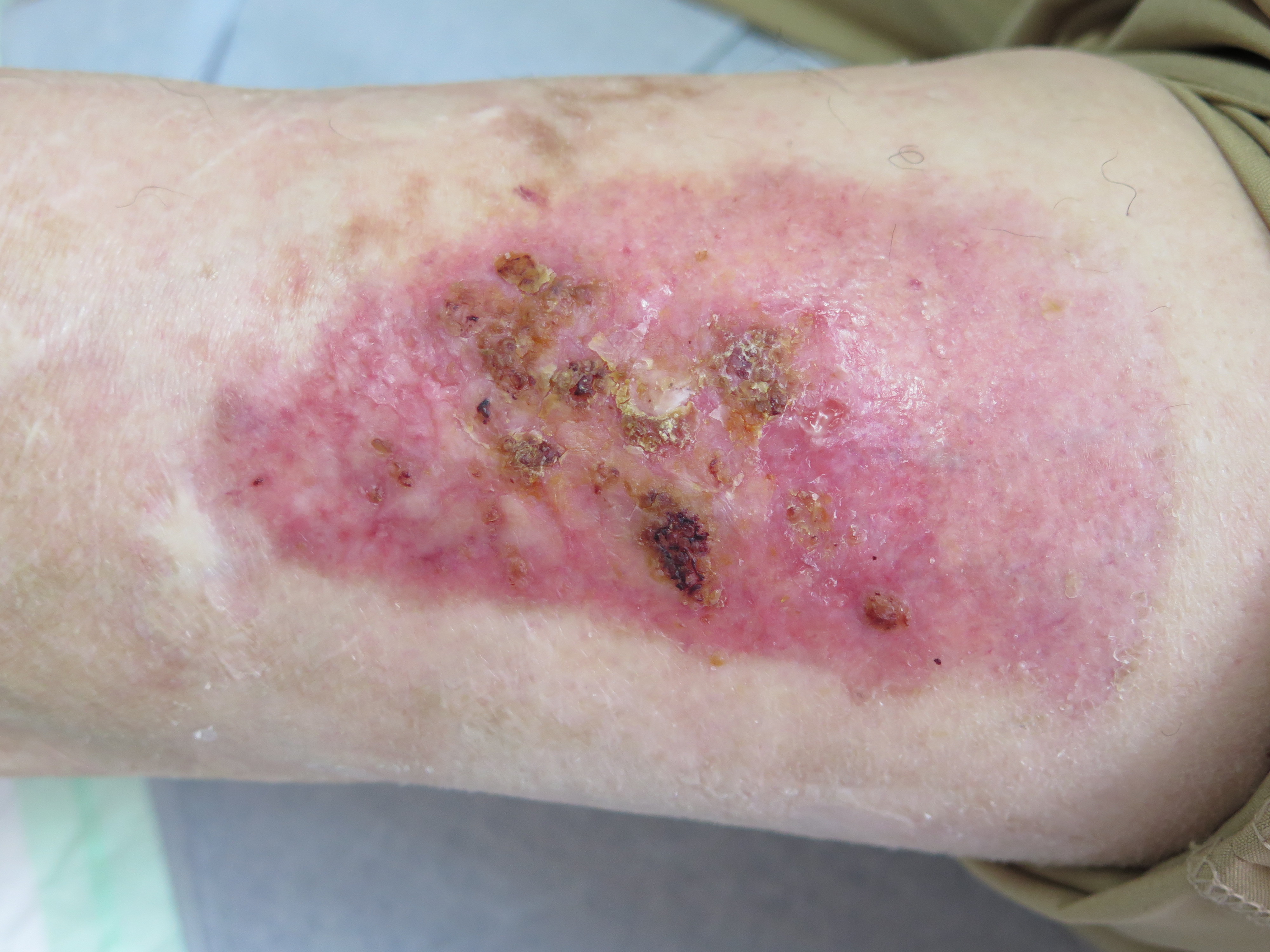
In this photo, erosions covered by crusts can be seen in the donor site for grafting (intervention performed 1 year before). The patient referred that the the clinical picture had started 15 days before with the arisal of pustules.
How is it diagnosed?
By performing a biopsy, we can observe erosions, subcorneal pustules and a non-specific dermal inflammatory infiltrate. When pustules are observed, they are not follicular (unlike bacterial folliculitis). There are usually no signs of vasculitis and no bacteria or fungi are observed.1
Microbiological culture tests are negative.
As we have seen, histological findings are not specific, but they help to rule out other diseases (inflammatory, infectious or tumoural) that may have a similar clinical presentation:2
- Irritative or allergic contact dermatitis
- Externaly triggered dermatitis (physical or chemical)
- Stasis eczema
- Erosions secondary to excessive exudate
- Bacterial folliculitis
- Pustular psoriasis
- Vegetative pyodermitis. It is produced by superficial abscesses due to staphylococcus or streptococcus.
- Superficial granulomatous pyoderma gangrenosum. These are erosions with raised edges. The biopsy shows a neutrophilic infiltration and vasculitis
- Bullous pemphigoid. It’s a type of self-immune bullous disease. Erosions occur after the formed blisters break. Direct immunofluorescence biopsy and the positivity of autoantibodies in the blood are key to its diagnosis
- Field cancerization (multiple actinic keratoses +/- squamous cell carcinoma, on atrophic skin with chronic sun damage).
How is it treated?
In the management of this disease, the failure of an adequate management with conventional dressings, compression, and local and systemic antibiotics is remarkable.
The treatment of choice is the use of a high-potency corticoid, covered by an interface and gauze, with variable frequency (initially daily application). I also use calcium alginate or pieces of zinc bandages. The treatment has to be maintained over time, an average of 3 months, and the frequency of application has to be progressively decreased. When treatment is stopped, up to half of the cases may recur.2
An alternative treatment is Tacrolimus 0.1%, with daily application. Resolution may take up to 16 weeks. Unlike topical steroids, it does not cause skin atrophy. It may be used in combination with topical steroid, scheduled after an initial course of topical steroid, or even used prophylactically twice a week to prevent recurrence.4
References
-
- Lanigan SW, Cotterill JA. Erosive pustular dermatosis: a common development in atrophic skin. Br J Dermatol 1987; 117: 15.
- Wantz M, Perceau G, Goeldel AL, Grange F, Bernard P. Erosive pustular dermatosis of the legs: retrospective study of 16 cases. Ann Dermatol Venereol. 2011;138(2):93–99.
- Patton D, Lynch PJ, Fung MA, Fazel N. Chronic atrophic erosive dermatosis of the scalp and extremities: a recharacterization of erosive pustular dermatosis. J Am Acad Dermatol. 2007;57(3):421–427
- Dall’Olio E, Rosina P, Girolomoni G. Erosive pustular dermatosis of the leg: long-term control with topical tacrolimus. Australas J Dermatol. 2011;52(1):e15–e17
Also available in: Español (Spanish)






