How many times have we asked ourselves this question, health professionals, caregivers and, of course, the people who suffer them on their own skin?
Without doubt, there are many ways of doing things (especially in the field of wound healing) and in most cases we don´t know which is the best alternative. However, in this type of ulcer, in older patients, with multiple comorbidities, the most frequent management is conservative, with the use of products that fail to promote healing and with the consequent associated complications (poor pain control, infections, hospitalization). The impact of these ulcers on the quality of life of elderly people is enormous. In many cases we find people over 90 years old, without any associated disease, to whom the onset of such a wound, after a mild traum, changes their lives. They stop walking, isolate themselves, become depressed, suffer unbearable pain that has to be treated with painkillers with many side effects…
As we commented in the post “Large leg ulcers after mild trauma”, age, hypertension and diabetes favour the process called arteriolosclerosis, which consists of the thickening and decrease in elasticity of the walls of the small arteries (arterioles), in some cases with the presence of calcifications. As I also explained in that post, arteriolosclerosis could be the trigger for the vicious necrosis-inflammation circle, which causes these large ulcers after minimal trauma.
Taking into account that we consider that Martorell ulcer and post-traumatic arteriolopathy associated to age share clinical aspects and both present arteriolosclerosis, we could consider both in the same disese spectrum that benefit from the same treatment, that is, punch grafting ?See post “Large leg ulcers after mild trauma”, Interest of early punch grafting in Martorell hypertensive ischemic ulcer”
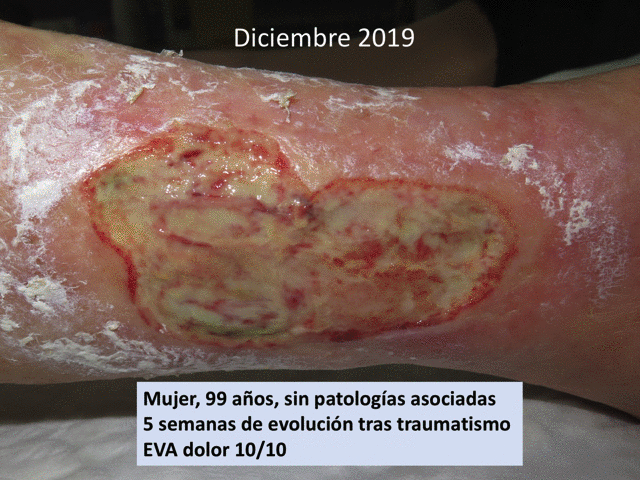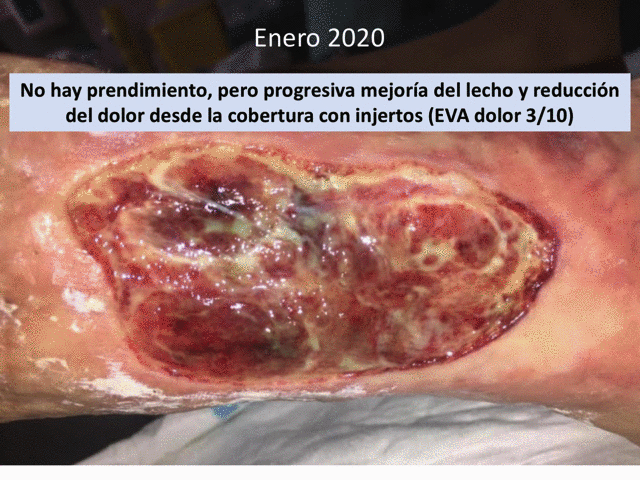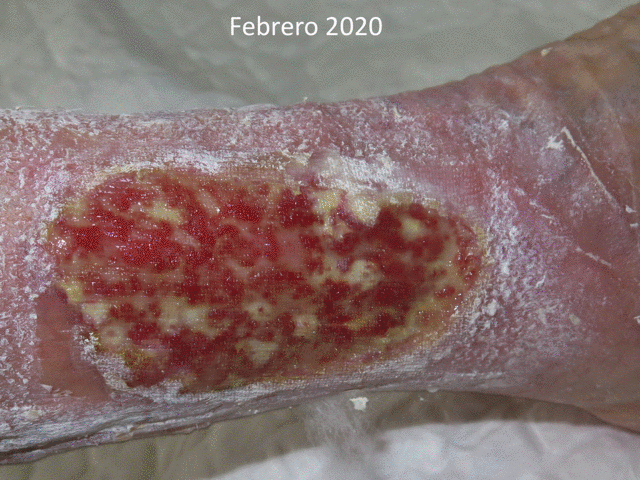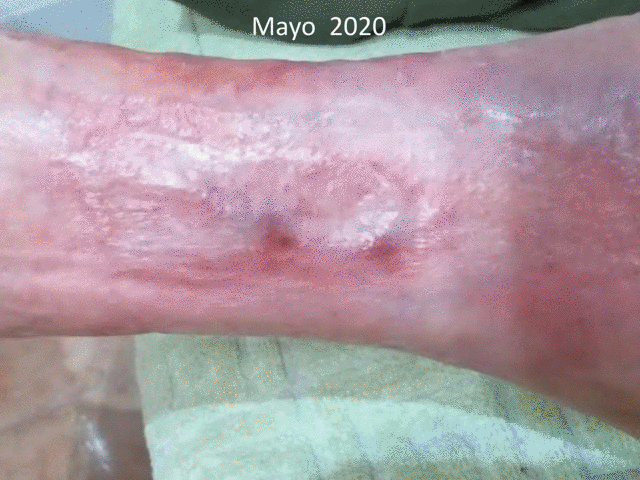
We always try to prepare the wound bed as well as possible to increase the percentage of graft taking. However, pain, often associated with a certain degree of cognitive impairment, makes adequate debridement difficult. Our solutions to this frequent problem are irrigation with sevoflurane, as an analgesic and vasodilator (“Have you ever heard of topical sevoflurane in wounds”) and early and sequential punch grafting in suboptimal beds. Sequential punch grafting (every 2-3 weeks) implies that with the first sessions we can achieve a progressive limitation of necrosis, wound contraction, decrease of pain and increase of granulation tissue, which will favour the attachment of subsequent grafts. That is, even if no graft gets attached on an initial bed with a lot of slough, this early coverage will promote the release of cells and growth factors essential for healing, in addition to having a significant analgesic effect (See post “Punch grafting as a painkiller for painful ulcers”)
Other allies in this anti-inflammatory and pro-epithelialisation strategy for these post-traumatic ulcers due to age-related arteriolopathy (which we also use for the Martorell ulcer) are:
- Topical corticosteroids (See post: “Interest of the topical corticosteroids in Martorell ulcer”)
- Zinc oxide (See post: “Why do we use topical zinc on wounds and perilesional skin? zinc oxide”)
- Negative pressure therapy (See post: “Punch grafting and negative pressure therapy: a successful couple”)
- Compression therapy adapted to the person’s comorbidities and tolerance, with other anti-edema measures.-Protection of the perilesional skin, which is essential as the elderly usually present skin fragility (See post “Wounds secondary to dermatoporosis or chronic venous insufficiency”)
I finish this post by sharing a case we have just published, which I hope you will find inspiring to help your patients 🙂
early and sequential punch grafting arteriolosclerosisAlso available in: Español (Spanish)






