The healing process of any leg wound is conditioned by gravity force.
The inflammatory process inherent in any leg wound involves an alteration in the microcirculation, with greater capillary filtration, and, due to the effect of gravity, an increase in intravenous pressure. Therefore, despite the absence of reflux or venous obstruction, a state of venous hypertension may develop, hindering healing. In this context, a post-traumatic or post-surgical leg injury will benefit from anti-gravity measures.
Therefore, compression therapy, which is both an essential anti-gravity and anti-inflammatory measure, is beneficial in this type of wounds, provided there is no contraindication.
– So let’s take the example of a young boy with no underlying venous pathology. Would he benefit from compression therapy after a leg injury due to either a fall or the removal of a melanocytic nevus?
– Yes, of course.
– Well, when should compression therapy be started?
– From the moment the wound occurs. Although, during the first few days, rest with the lower limb properly elevated is the most important anti-gravity recommendation, the placement of a compression bandage or compression stocking will help the patient return to normal activities earlier.
– And how long should compression therapy be maintained?
– Unlike cases of chronic venous insufficiency, these patients may stop wearing a compression bandage or stocking once the wound is closed, there are no signs of local inflammation and no oedema occurs after discontinuation of use.
After discussing the benefits of compression to promote healing of leg wounds, let’s talk about a strategy that can help improve the appearance and functionality of scars: massage.
Why, when and how to massage a scar? Is it a treatment that you recommend in your clinical practice?
First of all, considering the scarcity of studies and the consequent lack of evidence, it must be stressed that absolute recommendations on scar massage cannot be established.
Why?
Because scar massage can influence the final stage of scarring, called remodelling phase, to achieve a better aesthetic, functional and wellness result. During the remodelling phase, which can last for years, the production of collagen is normally reduced. These collagen fibres will be reorganised to try to achieve about 80% of the elasticity and strength of normal skin.
Excessive scar tissue can lead to a hypertrophic scar (red and raised tissue that worsens months after wound production and improves spontaneously in the next 1-2 years) or a keloid (it extends beyond the limits of the original wound and does not improve without treatment). To remember the phases of wound healing, you can read the post “Brief overview of wound healing“.
We will explain the hypotheses that have been proposed to explain the positive effects of massage on scar remodelling
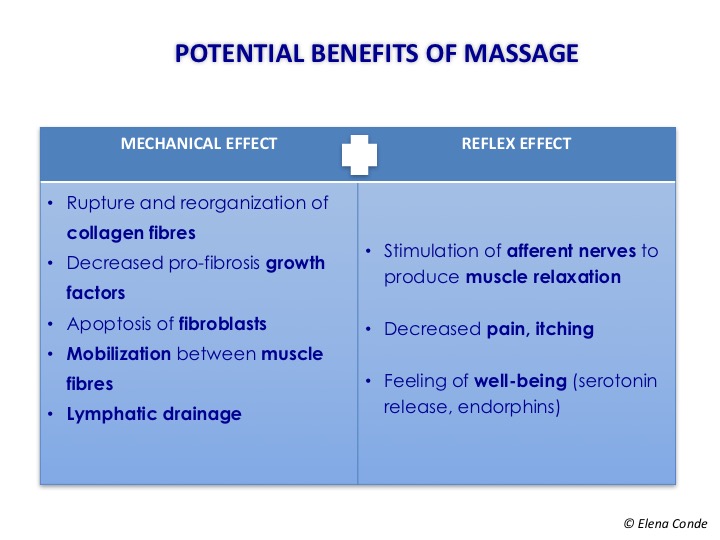
With respect to mechanical stimulation, massage forces can induce changes in the expression of extracellular matrix proteins, pro-fibrosis growth factors and proteases, with the consequent apoptosis of fibroblasts and lower collagen production.1 This limitation of fibrosis accelerates scar maturation, which is interesting for the prevention and treatment of hypertrophic wounds. Massage can decrease adhesion with deep tissues increase the elasticity of the scar. In addition, lymphatic drainage helps to decrease swelling and oedema.
On the other hand, in addition to its physical effect, by stimulating afferent nerve fibres, reflex muscle relaxation can be produced, as well as release of serotonin, beta-endorphins, and other neurotransmitters with consequent decreased pain and itching and improved mood.
A review2 conducted in 2011 brings together 10 studies, involving children and adults. These are case series and controlled trials with a small sample size (fewer than 25 patients in each group), which include predominantly burns or post-surgical wounds on the face and extremities. The results of these studies point to the potential benefit of massage in scar appearance and function, in addition to pain and itching reduction, and improvement in mood.
In a clinical trial3 published later, including 146 patients with hypertrophic burn scars, the benefit of massage, performed by a specialist for 30 minutes twice a week, was studied. The average time of evolution since the production of the burn was 5 months and massages were maintained an average of 1 month. When comparing the treatment group (76 patients) with the control group, a reduction in pruritus and pain on a visual analogue scale was observed. An improvement in wound characteristics was also observed, such as thickening, erythema, hyperpigmentation and scar distensibility. The positive results of a recent review4 to evaluate massage, specifically in hypertrophic burn scars, suggest that well-designed clinical trials are needed to develop evidence-based guidelines for scar massage.
When?
Once complete epithelialisation has been achieved, i.e. when the wound is closed, massage sessions can begin. In post-surgical wounds, after removal of the stitches, if total closure is observed. Massage in the early stages of healing is not indicated, as it may delay healing and increase the risk of hypertrophy.
Any type of wound can be treated with massage, although the most studied have been burns and post-surgical wounds.
In studies reported in the medical literature, start and end time of treatment, the frequency and duration of each massage is highly variable.2-4 In addition, the variables used to analyse the response to treatment of a scar have not been consensually defined and are mostly subjective. Bearing this in mind, it is difficult to compare the results of 30-minute treatments twice a week, performed by an expert, with a massage 10 minutes a day by the patient himself. It is also complicated to compare scars that are treated at different time points of their evolution (the benefit of massage has been described in wounds lasting less than one month to long-length scars).
The usual recommendation that is made to patients is a massage of 5-10 minute, twice a day.
If pain makes it difficult to manipulate the scar, short and less frequent massages can be performed.
Most studies analyse the response to massage limited in time, mostly between 1-3 months. Since the optimal duration of treatment is unknown, it would be recommended to maintain the massage until its benefits are no longer observed.
How?
There are different techniques. The most widespread recommendations to facilitate patient autonomy in treatment is to perform cycles with different movements, as shown in the drawing.
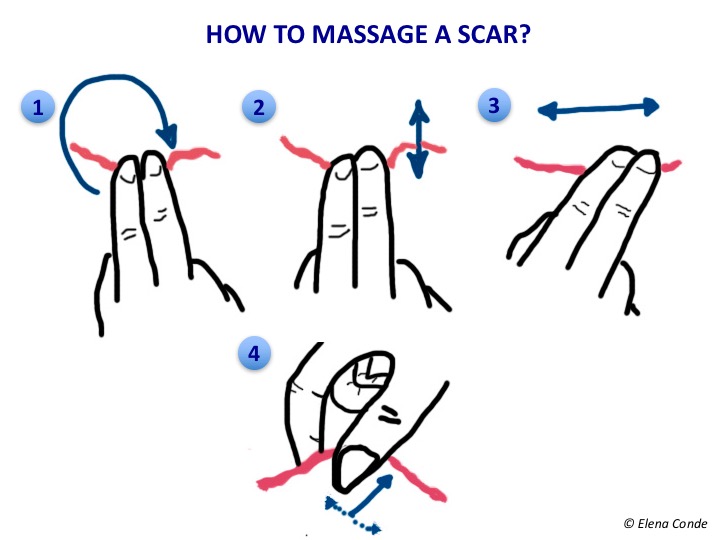
We would start with a circular rhythmic movement (Figure 1), with enough pressure to whiten the scar skin but avoiding friction on the epidermis so as not to damage it (we press and move the finger and skin at the same time). We can continue with parallel (Figure 2) and perpendicular (Figure 3) motions. Deep palpation of the scarred skin fold between the thumb and the second finger, called skin rolling, (Figure 4) helps to reduce fibrous adhesions between the skin and deep tissues.
It is widely recommended to perform the massage with a moisturizing product that facilitates the movement of the fingers without damaging the epidermis. Hypoallergenic products should be used to minimize the risk of contact dermatitis.
Do you usually recommend compression therapy for post-surgical or post-traumatic wounds? Do you have any experience with scar massage?
References:
Also available in: Español (Spanish)






