How many times have you heard “if a wound itches it is because it is healing”? Well, this popular belief has some truth to it, since itching is normal in the healing process and usually appears in the later stages. However, as we will see below, it occurs in both acute and chronic wounds, and even scars, and is mainly associated with the inflammatory process (pruritoceptive pruritus) or nerve damage (neuropathic pruritus), not necessarily with a good wound evolution.
Itching can be very bothersome and unresponsive to multiple treatments. This can have a great impact on people’s quality of life, especially when it is persistent in chronic wounds or scars.1-5
There are still many unknowns about the pathophysiology of wound pruritus, but in this post we will summarize the available evidence that helps us to better understand this very uncomfortable symptomatology.
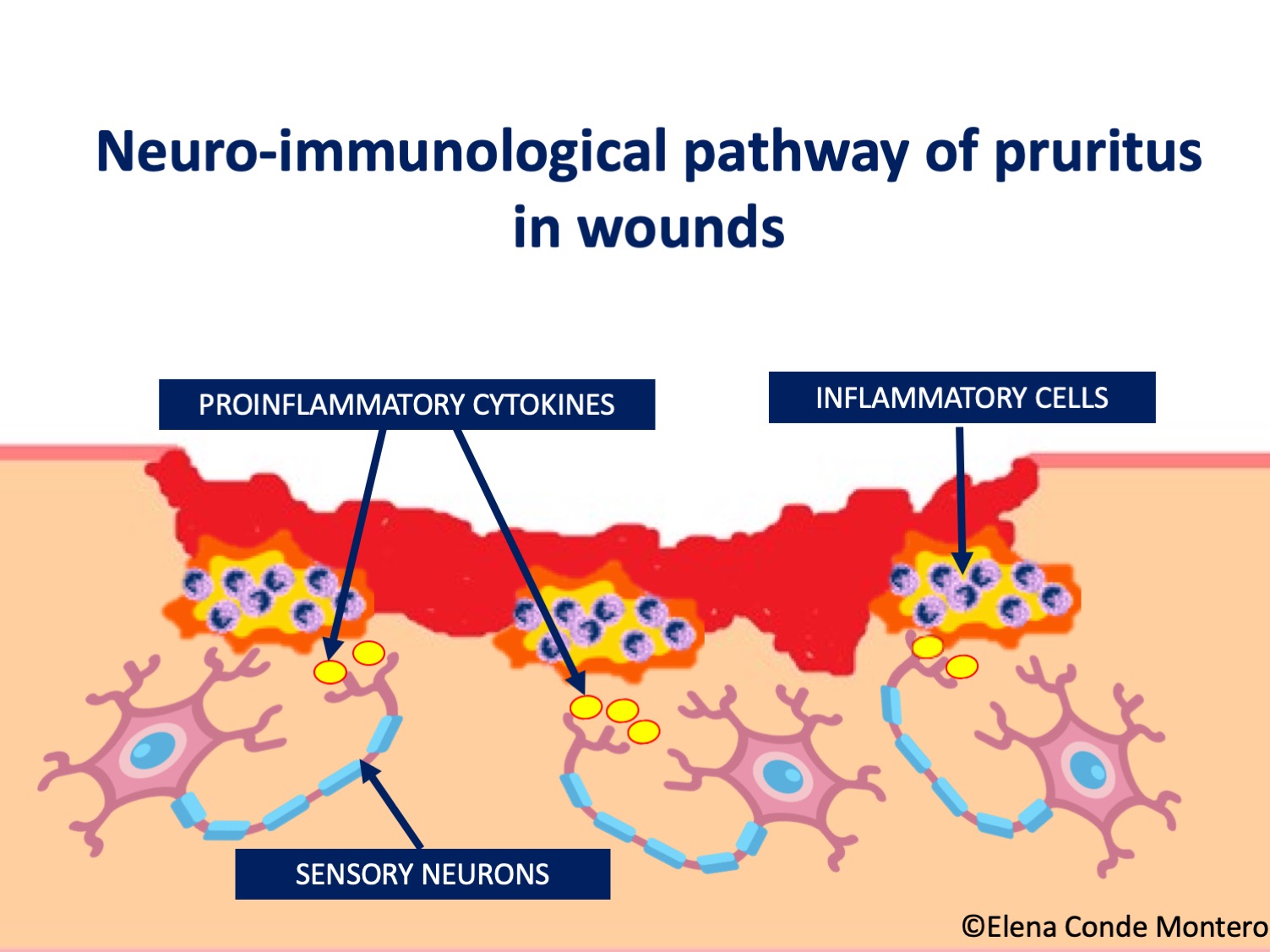
Proinflammatory cytokines released in any wound (acute or chronic) can activate sensory neurons and produce itching. This is termed the neuro-immunologic pathway of pruritus and multiple cells appear to be involved, including white blood cells, keratinocytes and endothelial cells.4 Pruritogenic molecules such as interleukin 31(IL-31)3 activate afferent sensory fibers in the skin and these neurons synapse with second-order neurons in the spinal cord. After communication with a complex of spinal interneurons, a signal is sent to the brain where the itch sensation is recognized. Instructions are then sent to the motor neurons responsible for scratching.
Microenvironmental factors also contribute to itching. These include dry scabs and perilesional deramatitis, as well as the presence of bacteria in the wound bed.
Histamine does not seem to be a clinically relevant contributor to wound-associated itching, so the interest of antihistamine use would be practically limited to its sedative effect.
A prospective study involving 200 chronic wounds of different etiologies (traumatic, pressure, neuropathic, venous, arterial, mixed and others) found that 28% of patients had wound-related pruritus. Lower extremity wounds were more likely to be itchy than upper body wounds and venous ulcers were significantly more itchy than other types of chronic wounds. Wound duration did not predict the occurrence of itching; however, pruritus was more prevalent in larger wounds, with edema, more granulation tissue or necrotic tissue.5
The persistence of pruritus after a burn is striking. The precise trigger for this phenomenon is unknown, but it seems that the neuropathic mechanism is the main one involved. In fact, these patients may report paresthesias (needle pricks). Neuropathic pruritus is due to increased sensitivity and excitability of damaged peripheral afferent fibers, which form neuromas. It may therefore respond to neuroleptic agents such as gabapentin and pregabalin.4
In pathologic scars following wounds with an intense inflammatory phase, i.e. hypertrophic and keloid scars, chronic pruritus is not uncommon. In keloids, abnormalities of afferent nerve fibers have also been reported, which could explain this itching.2
Proteomics and metabolomics studies will allow us to profile in more detail the mediators involved in wound itching and will help us understand why some wounds and scars itch and others do not. These data can then be used to develop targeted therapies for itch. Until then, wound itch treatment will remain poorly targeted.
References:
1. Lerner E. Why Do Wounds Itch? Wounds. 2018 Jan;30(1):1-3.
2. Parnell LKS. Itching for Knowledge About Wound and Scar Pruritus. Wounds. 2018 Jan;30(1):17-36.
5. Paul J. Characteristics of chronic wounds that itch. Adv Skin Wound Care. 2013;26(7):320–332. 53.
Also available in: Español (Spanish)






